Cancer vaccines
Most of us know about vaccines given to healthy people to help prevent infections, such as measles and mumps. These vaccines use weakened or killed germs like viruses or bacteria to start an immune response in the body. Getting the immune system ready to defend against these germs helps keep people from getting infections.
Most cancer vaccines work the same way, but they usually prime the immune system to attack cancer cells in the body. The goal is to help treat cancer or to help prevent it from coming back after other treatments. But there are some vaccines that may actually help prevent certain cancers.
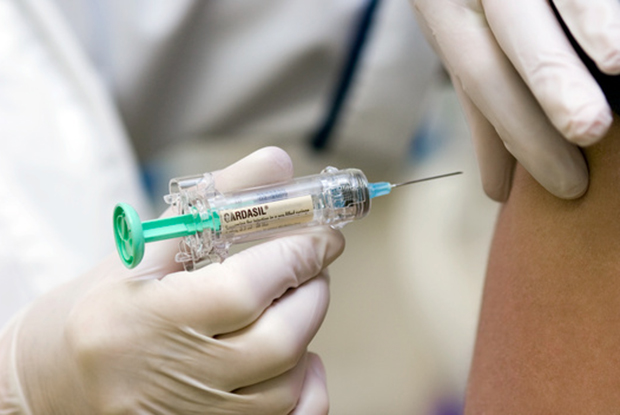
Vaccines to help prevent cancer
Many people might not realize it, but some cancersQ are caused by viruses. Vaccines that help protect against infections with these viruses might also help prevent some of these cancers.
Some strains of the human papilloma virus (HPV) have been linked to cervical, anal, throat, and some other cancers. Vaccines against HPV may help protect against some of these cancers.
People who have chronic (long-term) infections with the hepatitis B virus (HBV) are at higher risk for liver cancer. Getting the HBV vaccine to help prevent this infection may therefore lower some people’s risk of getting liver cancer.
These are traditional vaccines in that they target the viruses that can cause certain cancers. They may help protect against some cancers, but they don’t target cancer cells directly. These types of vaccines are only useful for cancers known to be caused by infections.
But most cancers, such as colorectal, lung, prostate, and breast cancers, are not thought to be caused by infections. Doctors are not yet sure if it will be possible to make vaccines to prevent these other cancers. Some researchers are now trying, but this research is still in very early stages. Even if such vaccines prove to be possible, it will be many years before they become available.
Vaccines to help treat cancer
Cancer treatment vaccines are different from the vaccines that work against viruses. These vaccines try to get the immune system to mount an attack against cancer cells in the body. Instead of preventing disease, they are meant to get the immune system to attack a disease that already exists.
A cancer treatment vaccine uses cancer cells, parts of cells, or pure antigens to increase the immune response against cancer cells that are already in the body. Vaccines are often combined with other substances or cells called adjuvants that help boost the immune response even further.
Cancer vaccines don’t just boost the immune system in general; they cause the immune system to attack cells with one or more specific antigens. And because the immune system has special cells for memory, it’s hoped that the drugs will help keep cancer from coming back.
Sipuleucel-T (Provenge®)
At this time, this is the only vaccine approved by the US Food and Drug Administration (FDA) to help treat cancer. It is used to treat advanced prostate cancer that is no longer being helped by hormone therapy.
The dendritic cells are then given back to the patient by infusion into a vein (IV). This process is repeated twice more, 2 weeks apart, so that the patient gets 3 doses of cells. Back in the body, the cells help other immune system cells attack the patient’s prostate cancer. Although the vaccine does not cure prostate cancer, it has been shown to help extend patient’s lives by several months on average. Studies to see if this vaccine can help men with less advanced prostate cancer are now being done.
Side effects are usually mild and can include fever, chills, fatigue, back and joint pain, nausea, and headache. A few men may have more severe symptoms, including problems breathing and high blood pressure.
Types of cancer treatment vaccines being studied
Several types of cancer vaccines are now being studied, with a few reaching late stage clinical trials.
Tumor cell vaccines:
These vaccines are made from actual cancer cells that have been removed during surgery. The cells are treated in the lab, usually with radiation, so they cannot form more tumors. In most cases, doctors also change the cells in certain ways, often by adding chemicals or new genes, to make them more likely to be seen as foreign by the immune system. The cells are then injected into the patient. The immune system recognizes antigens on these cells, then seeks out and attacks any other cells with these antigens that are still in the body.
Most tumor cell vaccines are autologous, meaning the vaccine is made from killed tumor cells taken from the same person in whom they will later be used. In other words, cells are taken from you (during surgery), the vaccine is made from them in a lab, and the cells are injected back into you. Some vaccines are allogeneic, meaning the cells for the vaccine come from someone other than the patient being treated. Allogeneic vaccines are easier to make than autologous vaccines, but it is not yet clear if one type is more effective than the other.
Antigen vaccines:
These vaccines boost the immune system by using only one antigen (or a few), rather than whole tumor cells that contain many thousands of antigens. The antigens are usually proteins or pieces of proteins called peptides.
Antigen vaccines may be specific for a certain type of cancer, but they are not made for a specific patient like autologous cell vaccines are. Scientists often combine several antigens in a vaccine to try to get a stronger immune response.
Dendritic cell vaccines:
Dendritic cells are special immune cells in the body that help the immune system recognize cancer cells. They break down cancer cells into smaller pieces (including antigens), then hold out these antigens so other immune cells called T cells can see them. This makes it easier for the immune system cells to recognize and attack cancer cells.
Dendritic cell vaccines are autologous vaccines (made from the person in whom they will be used), and must be made individually for each patient. The process used to create them is complex and expensive. Doctors remove some immune cells from the blood and expose them in the lab to cancer cells or cancer antigens, as well as to other chemicals that turn them into dendritic cells and help them grow. The dendritic cells are then injected back into the patient, where they should provoke an immune response to cancer cells in the body.
Sipuleucel-T (Provenge), which is used to treat advanced prostate cancer, is an example of a dendritic cell vaccine.
DNA vaccines:
When tumor cells or antigens are injected into the body as a vaccine, they may cause the desired immune response at first, but they may become less effective over time. This is because the immune system recognizes them as foreign and quickly destroys them. Without any further stimulation, the immune system often returns to its normal (pre-vaccine) state of activity. To get around this, scientists have looked for a way to provide a steady supply of antigens to keep the immune response going.
DNA is the substance in cells that contains the genetic code for the proteins that cells make. Vectors (see next section) can be given bits of DNA that code for protein antigens. When the vectors are then injected into the body, this DNA might be taken up by cells and can instruct them to make specific antigens, which would then provoke the desired immune response. These types of therapies are called DNA vaccines.
Vector-based vaccines:
These vaccines use special delivery systems (called vectors) to make them more effective. They aren’t really a separate category of vaccine; for example, there are vector-based antigen vaccines and vector-based DNA vaccines.
Vectors are special viruses, bacteria, yeast cells, or other structures that can be used to get antigens or DNA into the body. The vectors are often germs that have been altered to make sure they can no longer cause disease.
Vectors may be helpful in making vaccines for a number of reasons. First, they may be used to deliver more than one cancer antigen at a time, which may make the body’s immune system more likely to mount a response. Second, vectors such as viruses and bacteria may trigger their own immune responses from the body, which may help make the overall immune response even stronger. Finally, these vaccines may be easier and less expensive to make than some other vaccines.
